Introduction
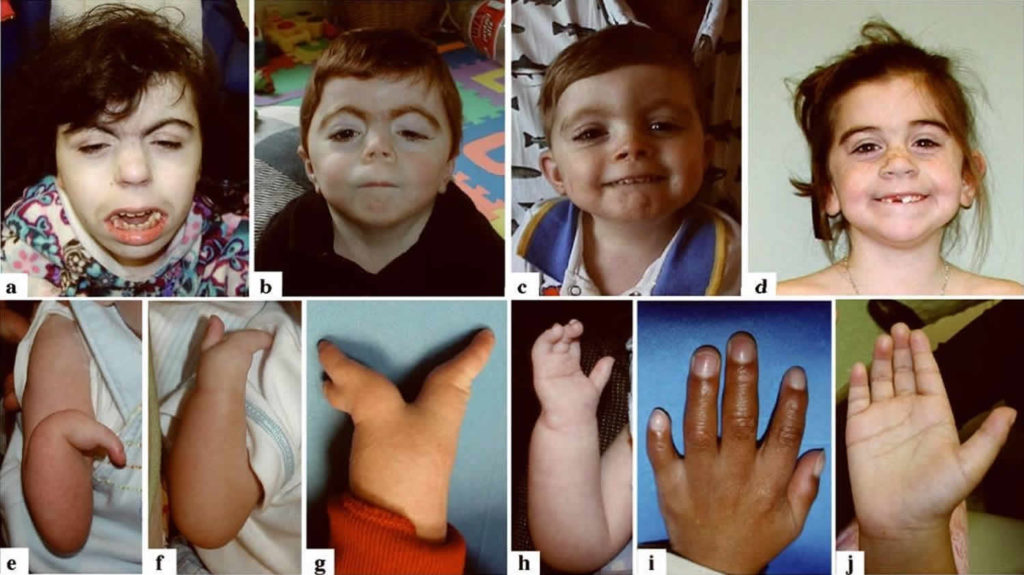
Medical Features and Pathophysiology
Etiology
CdLS is primarily caused by mutations affecting the cohesin complex, crucial for chromosomal segregation and gene regulation. NIPBL accounts for approximately 60% of cases, with SMC1A, SMC3, HDAC8, RAD21, ANKRD11, and BRD4 mutations responsible for the remainder. Most mutations arise de novo, though autosomal dominant and X-linked inheritance patterns occur.
Pathology
The syndrome presents with highly variable severity. Common features include growth delays, distinctive facial features (synophrys, long eyelashes, small upturned nose, thin downturned lips), limb abnormalities ranging from small hands to missing digits, intellectual disability, and behavioral challenges. Additional complications include hirsutism, gastroesophageal reflux, congenital heart defects, hearing loss, and vision problems.
Symptoms
- Growth Delays: Slow growth before and after birth, resulting in short stature.
- Distinctive Facial Features: Microcephaly, synophrys, long eyelashes, short upturned nose, thin downturned lips, low-set ears.
- Limb Abnormalities: Small hands and feet, clinodactyly, syndactyly, occasionally absent forearms or fingers.
- Intellectual Disability: Ranges from mild to severe with developmental delays and learning difficulties.
- Behavioral Issues: Autism spectrum disorders, attention deficits, hyperactivity.
- Medical Complications: Seizures, GERD, congenital heart defects, hearing loss, vision problems, dental issues.
Diagnosis
Diagnosis relies on clinical recognition of characteristic physical features and developmental delays. Genetic testing confirms the diagnosis by identifying mutations in associated genes. Prenatal diagnosis is possible through ultrasound and genetic testing with known family history.
Assistive Technology Suggestions and Requirements
Approximately 80-90% of individuals with CdLS require assistive technology. Communication needs vary widely with cognitive level and limb involvement. Many individuals benefit from symbol-based AAC, though significant upper limb abnormalities may necessitate switch or eye-gaze access.
Assistive Technology Suggestions
- Communication Devices: AAC devices essential for individuals with speech and language difficulties.
- Mobility Aids: Customized wheelchairs and mobility aids address physical impairments and coordination issues.
- Educational Tools: Tablets with specialized apps support cognitive development and learning.
- Environmental Control Systems: Enable control of environment using adaptive switches or voice commands.
Access Modalities
- Switch Access: Suitable for individuals with limited motor skills.
- Eye-Gaze Technology: Beneficial for severe motor impairments, though vision problems may limit candidacy.
- Touchscreen Devices: Appropriate for individuals with functional hand use, even if uncoordinated.
Care Management and Therapeutic Techniques
High Priority Goals
- Seizure Management: Control seizure frequency and severity through appropriate medications.
- Developmental Support: Maximize potential through early intervention targeting cognitive, motor, and communication skills.
- Daily Living Assistance: Support independence through assistive technologies and adaptive equipment.
- Family Support: Provide education, resources, and emotional support to families.
SLP Suggestions:
- Early Intervention: Initiating speech and language therapy as early as possible to support communication development. Early intervention programs should focus on developing basic communication skills, understanding, and social interactions.
- AAC Implementation: Introducing AAC devices tailored to the individual’s needs and capabilities is essential. Regular updates and customization of the device vocabulary ensure it remains relevant and useful.
- Oral Motor Therapy: Addressing feeding and swallowing difficulties through targeted exercises and strategies to improve oral motor function and safety. Techniques may include strengthening exercises, positioning strategies, and texture modifications.
- Family Training: Educating and involving family members in using AAC devices and communication strategies at home to ensure consistency and reinforcement. Providing resources and training sessions can empower families to support communication development effectively.
Special Educator Suggestions:
- Individualized Education Plan (IEP): Developing and regularly updating an IEP that includes specific goals and accommodations tailored to the student's strengths and needs. The IEP should address cognitive, motor, communication, and social-emotional development.
- Sensory Integration Therapy: Incorporating sensory activities that help with sensory processing issues, improving focus and engagement. Activities may include tactile play, movement exercises, and proprioceptive input.
- Inclusive Classroom Strategies: Utilizing visual supports, structured routines, and differentiated instruction to create an inclusive learning environment. Strategies such as visual schedules, social stories, and task analysis can enhance understanding and participation.
- Life Skills Training: Emphasizing the development of life skills that promote independence and daily living activities. This includes teaching self-care skills, social interactions, and functional communication.
Occupational Therapist Suggestions:
- Motor Skill Development: Implementing exercises and activities to improve fine and gross motor skills, enhancing overall physical functioning. Techniques may include hand strengthening exercises, coordination tasks, and mobility training.
- Adaptive Equipment: Recommending and training the use of adaptive equipment for daily tasks, such as specialized utensils, writing aids, and dressing aids. These tools can enhance independence and facilitate participation in daily activities.
- Sensory Processing: Addressing sensory processing issues through tailored sensory diets and activities that help regulate responses to sensory input. This may involve creating a sensory-friendly environment and incorporating sensory breaks into the daily routine.
- Positioning and Mobility: Ensuring proper positioning and support in wheelchairs and other seating systems to prevent deformities and promote comfort. Assessing and adapting the home and school environment to facilitate mobility and accessibility.
Recommendations on AAC:
- Symbol-Based Communication: For individuals with limited verbal abilities, using symbol-based communication systems such as picture boards or symbol-based AAC devices can be highly effective. These systems use visual symbols to represent words or concepts, facilitating communication.
- Text-Based Communication: For those who can read and write, text-based AAC devices can provide a more reliable communication platform. These devices allow users to type out messages, which can be spoken aloud by the device.
- Custom Vocabulary Sets: Customizing the AAC device with vocabulary sets that are meaningful and relevant to the individual’s daily life, activities, and preferences. This ensures the device is user-friendly and encourages active use.
- Ongoing Assessment: Regularly reassessing the individual’s communication needs and abilities to ensure the AAC system remains appropriate and effective. Adjustments and updates should be made as needed to support evolving communication goals.
Comprehensive Management and Care Strategies
Medical Management
- Seizure Control: Antiepileptic medications are the mainstay of treatment for managing seizures in individuals with CdLS. Commonly used medications include valproic acid, clonazepam, and lamotrigine. In some cases, dietary therapies such as the ketogenic diet may also be beneficial.
- Sleep Management: Sleep disturbances are common in CdLS. Behavioral interventions and medications such as melatonin can help improve sleep patterns.
- Gastrointestinal Care: Addressing feeding difficulties and gastrointestinal issues is critical. High-calorie formulas or gastrostomy tube feeding may be necessary for those with severe feeding problems.
- Monitoring and treating orthopedic issues such as scoliosis and hip dislocation is essential. Regular assessments by an orthopedic specialist and physical therapy can help manage these conditions.
Behavioral and Psychological Support
- Behavioral Interventions: Behavioral therapies, including Applied Behavior Analysis (ABA) and behavior modification strategies, are effective in managing hyperactivity, attention deficits, and other behavioral issues associated with CdLS.
- Psychological Support: Providing psychological support for both the individual and their family is crucial. Counseling and support groups can help families cope with the challenges of caring for a child with CdLS.
- Reinforcement Strategies: Positive reinforcement strategies can be used to encourage desired behaviors and skills, enhancing overall development and quality of life.
Therapies and Interventions
- Physical Therapy: Physical therapy focuses on improving motor skills, balance, and coordination. Regular sessions help in managing ataxia and promoting mobility.
- Occupational Therapy: Occupational therapy assists with daily living skills, sensory processing, and fine motor skills. It also involves recommending adaptive equipment to support independence.
- Speech and Language Therapy: Speech therapy is essential for developing communication skills. Introducing AAC devices and non-verbal communication methods early can significantly benefit individuals with CdLS.
- Hydrotherapy: Water-based therapies can improve muscle strength, coordination, and relaxation, making them a beneficial adjunct to traditional therapies.
- Vision and Hearing: Regular assessments by ophthalmologists and audiologists are important to address any visual or auditory impairments that may be present.
Educational Strategies
- Specialized Education Plans: Developing individualized education plans (IEPs) that cater to the specific needs of the child. These plans should be flexible and adaptable to the child's evolving capabilities and needs.
- Inclusion Strategies: Including children with CdLS in mainstream classrooms with appropriate supports can enhance social interactions and provide a more inclusive educational experience.
- Use of Technology: Integrating technology in education through tablets, interactive apps, and other digital tools can aid learning and engagement.
Family and Community Support
- Support Groups: Connecting with other families through support groups can provide emotional support, practical advice, and a sense of community.
- Respite Care: Providing families with access to respite care services can offer much-needed breaks, helping to prevent caregiver burnout.
- Advocacy and Resources: Educating families about available resources, advocacy organizations, and legal rights ensures they can access necessary services and support.
Challenges and Considerations
- Medical Challenges: Managing multiple medical issues, including seizures, sleep disturbances, and feeding difficulties, requires a coordinated approach involving various healthcare professionals.
- Educational Barriers: Ensuring that educational strategies are tailored to the child's unique learning needs and that educators are trained to support these needs effectively.
- Behavioral Issues: Addressing behavioral challenges such as hyperactivity and attention deficits through consistent behavioral strategies and therapeutic interventions.
- Social Integration: Promoting social interactions and inclusion within the community to enhance the individual's quality of life and prevent social isolation.
Future Directions and Research
- Genetic Research: Ongoing research into the genetic mechanisms underlying CdLS holds promise for future treatments and potential cures. Gene therapy and other advanced techniques are being explored.
- Clinical Trials: Participation in clinical trials can provide access to new treatments and therapies, contributing to the broader understanding of the syndrome and improving care.
- Therapeutic Innovations: Developing new therapeutic approaches, including targeted medications, advanced AAC technologies, and innovative behavioral interventions, to enhance the quality of life for individuals with CdLS.
Clinical Information
The following data is from validated clinical sources and patient registries.
Core Characteristics
- Etiology: Genetic
- Pathology: Mutation - De Novo
- Rarity Classification: Orphan
- Typical Onset: Birth
- Gender Impact: Either Gender
- Seizure Prevalence: Variable (Ideopathic)
- Population Trend: Unknown
Pathophysiology
NIPBL (majority); 10%: SMC1A, SMC3, HDAC8, RAD21
AAC Considerations
Recommended Access Modalities: All - Variable
Additional Clinical Notes
Often could be candidates for eye gaze but vision can be highly impacted. More likely a durable dedicated device via touch/switch; these numbers are highly generous in estimate of mortality.
Patient Advocacy & Support Organizations
References
- National Organization for Rare Disorders (NORD): Provides a thorough overview of Cornelia de Lange Syndrome, including signs, symptoms, and current research.
- Genetic and Rare Diseases Information Center (GARD): A resource for detailed information on rare diseases, including Cornelia de Lange Syndrome.
- Cornelia de Lange Syndrome Foundation: Offers comprehensive resources and support for individuals with Cornelia de Lange Syndrome and their families.
- Boston Children's Hospital: Detailed information on the symptoms, causes, and management of Cornelia de Lange Syndrome.
- MedlinePlus Genetics: Overview of Cornelia de Lange Syndrome, including genetic aspects and clinical features.
- Cleveland Clinic: Information on the symptoms, causes, and complications of Cornelia de Lange Syndrome.
Care Management and Therapeutic Techniques
- Aims:
- Symptom Management: Addressing specific symptoms, such as seizures, reflux, and behavioral issues, to improve quality of life.
- Developmental Support: Maximizing developmental potential through early and ongoing interventions focusing on cognitive, motor, and communication skills.
- Daily Living Assistance: Providing support for activities of daily living to enhance independence and quality of life through the use of assistive technologies and adaptive equipment.
- Family Support: Offering education, resources, and emotional support to families to help them navigate the challenges associated with CdLS, ensuring a supportive home environment.
SLP Suggestions:
- Early Intervention: Initiating speech and language therapy as early as possible is crucial to support communication development, even if the individual is non-verbal. Early intervention focuses on developing pre-linguistic skills, such as joint attention, turn-taking, and symbolic play, which lay the foundation for later communication development. [2]
- AAC Implementation: Introducing and customizing AAC devices tailored to the individual’s needs and capabilities is essential. This involves selecting the appropriate type of device, customizing vocabulary sets, and providing ongoing training and support to ensure effective use of the AAC system. [2]
- Oral Motor Therapy: Addressing feeding and swallowing difficulties through targeted exercises and strategies is important to improve oral motor function and safety. Techniques may include strengthening exercises, positioning strategies, and texture modifications to facilitate safe and efficient feeding.
- Family Training: Educating and involving family members in using AAC devices and communication strategies at home is crucial to ensure consistency and reinforcement. Providing resources and training sessions can empower families to support communication development effectively in everyday interactions.
Special Educator Suggestions:
- Individualized Education Plan (IEP): Developing and regularly updating an IEP that includes specific goals and accommodations tailored to the student's strengths and needs is essential. The IEP should address cognitive, motor, communication, and social-emotional development, providing a roadmap for educational progress. [6]
- Sensory Integration Therapy: Incorporating sensory activities into the educational program can help with sensory processing issues, improving focus and engagement. Activities may include tactile play, movement exercises, and proprioceptive input, tailored to the individual's sensory profile.
- Inclusive Classroom Strategies: Utilizing visual supports, structured routines, and differentiated instruction can create an inclusive learning environment that supports the student's participation and success. Strategies such as visual schedules, social stories, and task analysis can enhance understanding and reduce anxiety.
- Life Skills Training: Emphasizing the development of life skills that promote independence and daily living activities is crucial. This includes teaching self-care skills, social interactions, and functional communication, preparing the individual for greater independence and community participation.
Occupational Therapist Suggestions:
- Motor Skill Development: Implementing exercises and activities to improve fine and gross motor skills is essential for enhancing overall physical functioning. Techniques may include hand strengthening exercises, coordination tasks, and mobility training, adapted to the individual's abilities and challenges.
- Adaptive Equipment: Recommending and training the use of adaptive equipment for daily tasks can enhance independence and facilitate participation in activities. This may include specialized utensils, writing aids, dressing aids, and other tools that support self-care and daily living skills.
- Sensory Processing: Addressing sensory processing issues through tailored sensory diets and activities can help regulate responses to sensory input, improving focus, behavior, and overall well-being. This may involve creating a sensory-friendly environment and incorporating sensory breaks into the daily routine.
- Positioning and Mobility: Ensuring proper positioning and support in wheelchairs and other seating systems is crucial to prevent deformities and promote comfort. Assessing and adapting the home and school environment to facilitate mobility and accessibility can enhance independence and participation.
Recommendations on AAC:
- Symbol-Based Communication: For individuals with limited verbal abilities, using symbol-based communication systems, such as picture boards or symbol-based AAC devices, can be highly effective. These systems use visual symbols to represent words or concepts, facilitating communication and expression.
- Text-Based Communication: For those who can read and write, text-based AAC devices can provide a more reliable communication platform. These devices allow users to type out messages, which can be spoken aloud by the device, enabling more complex and nuanced communication.
- Custom Vocabulary Sets: Customizing the AAC device with vocabulary sets that are meaningful and relevant to the individual's daily life, activities, and preferences is essential. This ensures the device is user-friendly and encourages active use, promoting communication success.
- Ongoing Assessment: Regularly reassessing the individual's communication needs and abilities is crucial to ensure the AAC system remains appropriate and effective. Adjustments and updates should be made as needed to support evolving communication goals and maximize communication potential.
Comprehensive Management and Care Strategies
Medical Management
- Growth Monitoring: Regular monitoring of growth and development is essential to identify and address any growth delays or nutritional deficiencies. Growth hormone therapy may be considered in some cases to improve growth outcomes.
- Cardiac Care: Individuals with CdLS may have congenital heart defects, requiring regular monitoring and management by a cardiologist. Medical or surgical interventions may be necessary to address heart problems and prevent complications.
- Gastrointestinal Management: Addressing gastrointestinal issues, such as reflux, constipation, and feeding difficulties, is crucial to ensure adequate nutrition and prevent complications. This may involve dietary modifications, medications, or, in severe cases, gastrostomy tube feeding.
- Orthopedic Care: Limb abnormalities and skeletal malformations may require orthopedic interventions, such as bracing, surgery, or physical therapy, to improve function and mobility.
- Sensory Impairments: Regular assessments by ophthalmologists and audiologists are essential to address any visual or auditory impairments that may be present. Vision therapy, hearing aids, or cochlear implants can be beneficial in improving sensory function and supporting development.
Behavioral and Psychological Support
- Behavioral Therapy: Behavioral therapies, such as Applied Behavior Analysis (ABA), can be effective in managing behavioral challenges, including hyperactivity, impulsivity, and self-injurious behaviors. These therapies focus on reinforcing desired behaviors and reducing problematic ones through structured interventions and positive reinforcement strategies.
- Psychological Support: Providing psychological support for both the individual and their family is crucial. Counseling and support groups can help families cope with the emotional and psychological challenges of caring for a child with CdLS. Connecting with other families who share similar experiences can provide a sense of community and support.
Therapies and Interventions
- Physical Therapy: Physical therapy focuses on improving motor skills, balance, and coordination. Regular sessions can help individuals with CdLS achieve greater mobility, improve muscle strength, and enhance their ability to participate in daily activities.
- Occupational Therapy: Occupational therapy assists with daily living skills, sensory processing, and fine motor skills. Therapists work with individuals to improve their ability to perform self-care tasks, such as dressing, feeding, and grooming. They may also recommend adaptive equipment to support independence and participation in daily activities.
- Speech-Language Therapy: Speech therapy is essential for developing communication skills, even if the individual is non-verbal. Therapists focus on alternative and augmentative communication (AAC) methods, such as sign language, picture exchange systems, or speech-generating devices, to enable individuals to express their needs and thoughts.
- Developmental Therapies: Early intervention programs and other developmental therapies can be beneficial in addressing developmental delays and supporting learning. These programs typically involve a team of specialists, including developmental pediatricians, therapists, and educators, who work together to create individualized plans to address the child's specific needs.
Educational Strategies
- Specialized Education Plans: Developing individualized education plans (IEPs) that cater to the specific needs of the child is crucial. These plans should be flexible and adaptable to the child's evolving capabilities and needs, addressing their unique learning style, strengths, and challenges.
- Inclusion Strategies: Including children with CdLS in mainstream classrooms with appropriate supports can enhance social interactions and provide a more inclusive educational experience. This may involve providing assistive technology, visual supports, and individualized instruction to support the student's participation and success.
- Use of Technology: Integrating technology in education through tablets, interactive apps, and other digital tools can aid learning and engagement. Educational software can be adapted to the individual's learning style and abilities, providing engaging and interactive learning experiences.
Family and Community Support
- Support Groups: Connecting with other families through support groups can provide emotional support, practical advice, and a sense of community. Sharing experiences, resources, and coping strategies with other families facing similar challenges can be invaluable. [2]
- Respite Care: Providing families with access to respite care services can offer much-needed breaks from the demands of caregiving. Respite care can help prevent caregiver burnout and allow families to attend to their own needs, improving their overall well-being. [4]
- Advocacy and Resources: Educating families about available resources, advocacy organizations, and legal rights ensures they can access necessary services and support. This may include information on financial assistance programs, educational advocacy, and legal guardianship.
Challenges and Considerations
- Medical Complexity: Managing multiple medical issues, including congenital heart defects, gastrointestinal problems, hearing loss, and vision problems, requires a coordinated approach involving various healthcare professionals. Coordinating care among specialists can be challenging, and families may need support in navigating the healthcare system.
- Communication Barriers: Speech and language delays can significantly impact communication and social interaction. Implementing effective AAC strategies and ensuring that communication partners are trained to support the individual's communication attempts is crucial.
- Behavioral Challenges: Behavioral problems, such as hyperactivity, impulsivity, and self-injurious behaviors, can pose significant challenges for families and caregivers. Developing a comprehensive behavior management plan that includes positive reinforcement, structured routines, and appropriate interventions is essential.
- Long-term Care: Individuals with CdLS often require lifelong support and supervision, placing significant demands on families and caregivers. Planning for long-term care needs, including residential options, financial planning, and legal guardianship, is essential.
Differential Diagnosis
Cornelia de Lange Syndrome shares some clinical features with other genetic disorders, making differential diagnosis crucial for appropriate management and genetic counseling. Conditions that may present with similar symptoms include:
- Rubinstein-Taybi Syndrome: Both disorders share features like broad thumbs and toes, intellectual disability, and distinctive facial features. However, Rubinstein-Taybi Syndrome is caused by mutations in the CREBBP or EP300 genes and has a different pattern of associated symptoms.
- Fetal Alcohol Spectrum Disorders (FASDs): Prenatal alcohol exposure can cause a range of physical, cognitive, and behavioral problems, including growth delays, facial abnormalities, and intellectual disability. However, FASDs are not genetic disorders and have a different etiology.
- Other Cohesinopathies: Several other disorders are caused by mutations in genes involved in the cohesin complex, such as Roberts Syndrome and Warsaw Breakage Syndrome. These disorders share some features with CdLS but have distinct clinical presentations and genetic causes.
Future Directions and Research
- Genetic Research: Ongoing research into the genetic mechanisms underlying CdLS holds promise for future treatments and potential cures. Advances in gene therapy and other cutting-edge techniques are being explored to address the root causes of the disorder. Researchers are working to understand how mutations in cohesin complex genes affect gene expression, cell division, and development, paving the way for targeted therapies.
- Clinical Trials: Participation in clinical trials can provide access to new treatments and therapies, contributing to the broader understanding of the syndrome and improving care. Researchers are continually seeking participants for studies aimed at developing and testing new interventions, including medications, therapies, and assistive technologies.
- Therapeutic Innovations: Developing new therapeutic approaches, including targeted medications, advanced AAC technologies, and innovative behavioral interventions, to enhance the quality of life for individuals with CdLS. Researchers are exploring various pharmacological and non-pharmacological treatments that may address specific symptoms and improve overall functioning.
- Understanding Genotype-Phenotype Correlations: Research is ongoing to better understand the relationship between specific gene mutations and the clinical presentation of CdLS. This knowledge will help clinicians predict the course of the disorder and tailor interventions to individual needs.
- Developing Targeted Therapies: Gene therapy approaches are being explored as a potential treatment for CdLS. These approaches aim to deliver a functional copy of the affected gene to cells, restoring normal gene expression and function. Other therapeutic strategies may focus on modulating downstream pathways affected by cohesin complex dysfunction.
- Improving Symptom Management: Research is ongoing to identify more effective medications and therapies to manage seizures, gastrointestinal issues, behavioral challenges, and other symptoms associated with CdLS. This includes exploring new anticonvulsant medications, developing novel therapies for reflux and constipation, and refining behavioral interventions to address specific challenges.
- Enhancing Communication and Social Interaction: Research is needed to develop and evaluate AAC interventions that are specifically tailored to the needs of individuals with CdLS. This includes exploring the use of eye-gaze technology, developing communication strategies that incorporate the individual's unique behavioral profile, and promoting social interaction skills.
- Supporting Families and Caregivers: Research is needed to identify effective support services for families and caregivers of individuals with CdLS. This includes developing interventions to address caregiver burden, providing access to respite care, and offering educational and emotional support.
Epidemiology and Demographics
Etiology and Pathophysiology
What causes Cornelia de Lange Syndrome?
What does Cornelia de Lange Syndrome do to the body?
Clinical Features and Stages
Diagnosis
Diagnostic Criteria
Genetic Testing
Differential Diagnosis
Assistive Technology and AAC Interventions
Communication Devices
Mobility Aids
Access Modalities
Environmental Control Units
Clinical Recommendations
For Speech-Language Pathologists
For Occupational Therapists
For Physical Therapists
For Applied Behavior Analysts
For Special Educators
For All Staff and Caregivers
Care Management
Medical Management
Positioning and Handling
Feeding and Swallowing
Psychosocial Support
Educational Support
IEP Goal Examples
Accommodations and Modifications
Transition Planning
Support and Resources
🏛️ Foundations and Research
🌐 Online Communities
📚 Educational Resources
💰 Financial Assistance
References
Disclaimer: This comprehensive clinical guide is designed for healthcare professionals, educators, and families. For specific medical advice, please consult with qualified healthcare providers.