Introduction
Progressive Supranuclear Palsy (PSP) is a rare neurodegenerative disorder typically affecting individuals in their late middle age to early elderly years, with a slightly higher prevalence in men. The disease is characterized by the gradual deterioration of specific brain areas, leading to motor and cognitive impairments. Diagnosis is based on clinical evaluation and characteristic symptoms, with imaging studies providing additional insights. Management of PSP involves a multidisciplinary approach, with a focus on maintaining independence and quality of life. Assistive technology, therapeutic interventions, and home modifications play a crucial role in managing symptoms. Speech-language pathologists, occupational therapists, and special educators provide essential support in managing the disease. Ongoing research into the disease's underlying mechanisms and potential treatments offers hope for future advancements in PSP care.
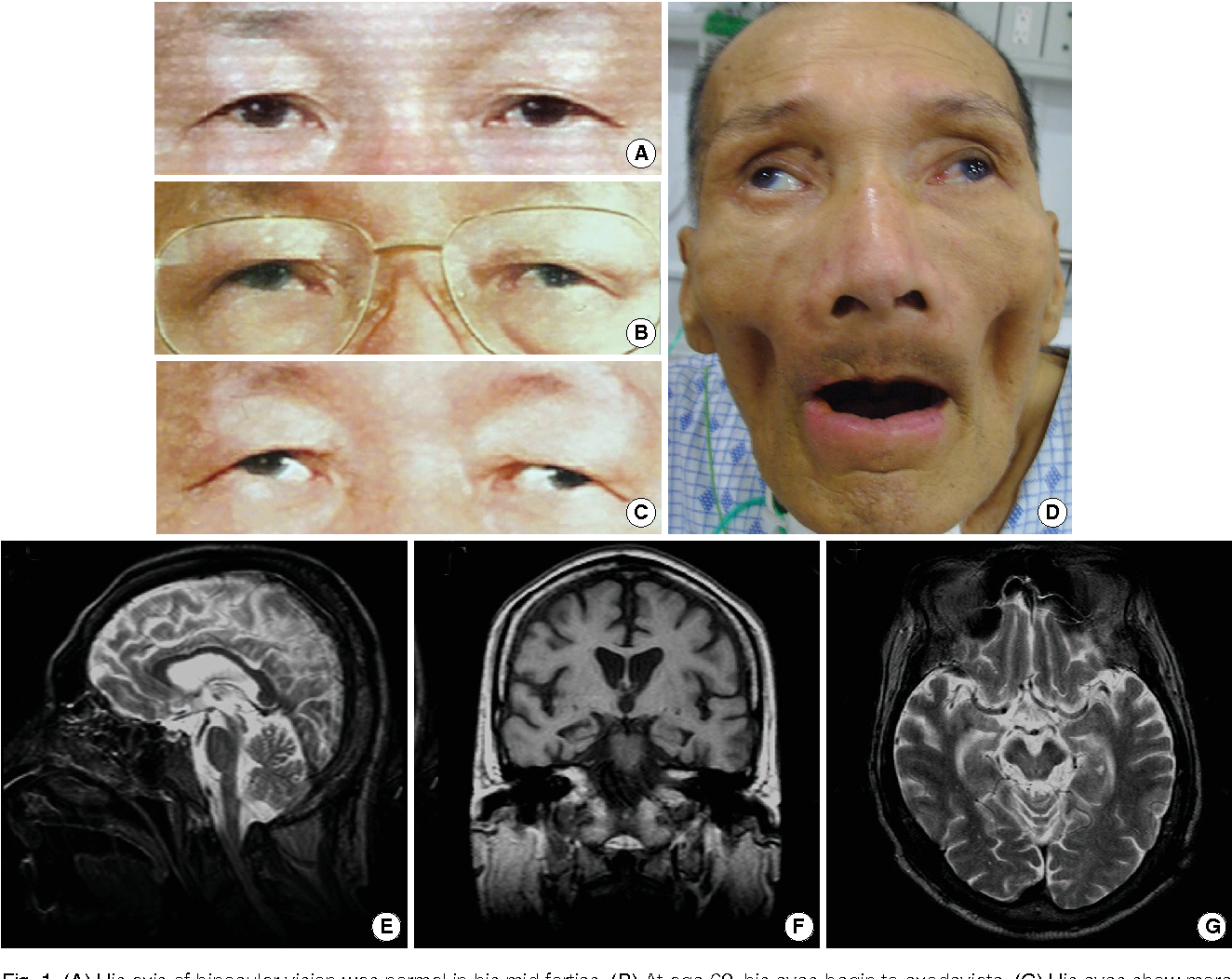
Progressive Supranuclear Palsy (PSP)
Demographic Information
- Incidence: Approximately 5-6 cases per 100,000 people
- Prevalence: Estimated 3-6 cases per 100,000 people
- Gender: Slightly more common in males (male-to-female ratio approximately 1.5:1)
- Onset Age: Typically begins in the late 50s to early 60s
Progressive Supranuclear Palsy (PSP) is an uncommon neurodegenerative disorder that generally affects individuals in their late middle age to early elderly years. The condition is slightly more prevalent in men than in women, and its onset commonly occurs in the late 50s to early 60s. The incidence and prevalence rates of PSP are relatively low, with approximately 5-6 cases diagnosed per 100,000 people. This rarity can sometimes lead to challenges in timely and accurate diagnosis.
Coding
- ICD-11: 8A06.0
- ICD-10-CM: G23.1
- OMIM: 601104
- UMLS: C0023492
- MeSH: D020534
- GARD: 7220
Progressive Supranuclear Palsy is classified under various medical coding systems that are used internationally to facilitate accurate diagnosis, research, and treatment. The International Classification of Diseases, 11th Revision (ICD-11) assigns PSP the code 8A06.0. The Online Mendelian Inheritance in Man (OMIM) database, which catalogues human genes and genetic disorders, lists PSP under the code 601104. The Unified Medical Language System (UMLS) includes PSP with the code C0023492, while the Medical Subject Headings (MeSH) term for PSP is D020534. Lastly, the Genetic and Rare Diseases Information Center (GARD) identifies PSP with the code 7220.
Medical Features and Pathophysiology
Etiology
Progressive Supranuclear Palsy (PSP) is a rare, neurodegenerative disorder characterized by the gradual deterioration of specific areas in the brain. The exact cause of PSP remains unknown, but it is believed to involve the accumulation of abnormal tau protein in brain cells, leading to cell damage and death. Genetic factors and environmental influences may also play a role, although no single genetic mutation has been definitively linked to PSP.
Pathology
PSP primarily affects the brainstem, basal ganglia, and cerebral cortex, leading to a variety of motor and cognitive impairments. The hallmark pathological feature is the presence of neurofibrillary tangles composed of tau protein, which disrupts normal cell function. This protein buildup is particularly evident in the brainstem, which controls eye movements and posture, contributing to the characteristic symptoms of the disease.
Symptoms
Early Symptoms
- Balance and gait disturbances, often leading to falls
- Bradykinesia (slowness of movement)
- Stiffness and rigidity in muscles
- Blurred or double vision due to difficulties in moving the eyes up and down (vertical gaze palsy)
Progressive Symptoms
- Severe difficulties with balance and coordination
- Dysphagia (difficulty swallowing)
- Dysarthria (difficulty speaking)
- Cognitive impairments, including problems with attention, planning, and executive function
- Emotional and behavioral changes, such as apathy, depression, and irritability
Diagnosis
PSP is diagnosed based on clinical evaluation and the presence of characteristic symptoms. There is no specific test for PSP, but imaging studies like MRI can reveal changes in the brain's structure, particularly atrophy in the midbrain. Positron Emission Tomography (PET) scans can help in identifying tau protein deposits. Neurological examination typically reveals abnormalities in eye movement, rigidity, and balance.
Assistive Suggestions and Requirements
Requirement Percentage for Assistive Technology
Progressive motor and cognitive impairments in PSP make assistive technology essential for nearly all patients as the disease advances.
Assistive Technology Suggestions
- Mobility Aids:
- Rollators or Walkers: To assist with walking and prevent falls.
- Wheelchairs: For advanced stages when walking becomes too difficult.
- Communication Aids:
- Voice Amplifiers: For speech that becomes soft or difficult to understand.
- Speech Generating Devices (SGDs): For those who lose the ability to speak clearly.
- Home Modifications:
- Grab Bars and Handrails: To enhance safety in bathrooms and along stairways.
- Adjustable Beds and Reclining Chairs: To facilitate ease of movement and comfort.
- Feeding Aids:
- Adaptive Utensils and Plates: For reduced dexterity.
Access Modalities
- Switch Access: For severe motor impairments to control communication devices and computers.
- Eye-Tracking Systems: For those who retain eye movement control but have lost most other motor functions.
- Touchscreen Devices: Useful in earlier stages when fine motor skills are relatively preserved.
Care Management and Therapeutic Techniques
Aims
- Maintain the highest possible level of independence and quality of life.
- Manage symptoms effectively through a multidisciplinary approach.
- Provide support and education to patients and caregivers.
SLP Suggestions
- Assessment and Intervention:
- Regular Speech and Swallowing Assessments: Monitor changes and adjust therapy plans.
- Swallowing Techniques: Ensure safe swallowing and reduce aspiration risk.
- Voice Therapy: Exercises to maintain voice strength and clarity.
- Augmentative and Alternative Communication (AAC):
- Early introduction of AAC devices ensures familiarity as communication abilities decline.
Special Educator Suggestions
- Cognitive Rehabilitation:
- Activities to enhance executive function, memory, and attention.
- Memory aids such as notebooks or electronic organizers.
- Behavioral Strategies:
- Structured routines to manage apathy and maintain engagement.
- Positive reinforcement to encourage participation and effort.
Occupational Therapist Suggestions
- Daily Living Skills:
- Training in adaptive equipment for self-care activities (dressing, grooming).
- Techniques to conserve energy and manage fatigue.
- Home and Environmental Modifications:
- Assess and modify the home environment for safety and accessibility.
- Recommendations for ergonomic furniture and tools to support independence.
Recommendations on AAC and Other Details
AAC selection depends on preserved cognitive and motor abilities. Individuals with PSP who maintain literacy benefit from text-based systems with predictive text to compensate for motor slowing. As cognitive impairments emerge, symbol-based approaches may become more appropriate.
- Text-Based AAC:
- Text-to-speech apps and devices for individuals who retain good literacy skills.
- Predictive text features to speed up communication.
- Symbol-Based AAC:
- Symbol-based systems like Picture Communication Symbols (PCS) for cognitive impairments affecting literacy.
- Dynamic display devices that adapt with the user's needs.
Clinical Information
The following data is from validated clinical sources and patient registries.
Core Characteristics
- Etiology: Genetic
- Pathology: Mutation - Somatic
- Rarity Classification: Rare
- Typical Onset: Adulthood
- Gender Impact: Either Gender
- Progressive/Degenerative: Yes
- Seizure Prevalence: No (<10%)
- Population Trend: Unknown
Pathophysiology
MAPT gene, and particularly its impact on microtubules and tau proteins, seem implicated but this is unproven. There is however some measure of familial association, although it's uncommon
AAC Considerations
Recommended Access Modalities: All - Progression
Additional Clinical Notes
Parkinsonslike in presentation but a bit more extreme in progression and emotional state.
Patient Advocacy & Support Organizations
References
- Boxer, A. L., & Lang, A. E. (2014). Progressive supranuclear palsy and corticobasal degeneration. Handbook of Clinical Neurology, 123, 611-631.
- Litvan, I., Agid, Y., Calne, D., Campbell, G., Dubois, B., & Duvoisin, R. C. (1996). Clinical research criteria for the diagnosis of progressive supranuclear palsy (Steele-Richardson-Olszewski syndrome): report of the NINDS-SPSP international workshop. Neurology, 47(1), 1-9.
- Williams, D. R., & Lees, A. J. (2009). Progressive supranuclear palsy: clinicopathological concepts and diagnostic challenges. The Lancet Neurology, 8(3), 270-279.
Additional Information
PSP is a complex and challenging condition that requires a coordinated approach to care. Regular follow-ups with a neurologist, along with support from a multidisciplinary team including speech-language pathologists, occupational therapists, and special educators, are essential for managing the disease. Patient and caregiver education, along with community resources and support groups, can provide valuable assistance in navigating the course of this progressive disorder.
For further information and support, patients and caregivers can refer to organizations such as the CurePSP Foundation (www.psp.org) and the PSP Association (www.pspassociation.org.uk), which offer resources, support networks, and advocacy for individuals affected by Progressive Supranuclear Palsy.
Extended Information
Pathological Insights and Disease Mechanism
The pathophysiological process underlying PSP is primarily driven by the accumulation of tau protein in neurons and glial cells. The tau protein, which normally stabilizes microtubules in neurons, becomes hyperphosphorylated and aggregates into neurofibrillary tangles. These tangles disrupt normal cell functions and lead to cell death. This pathological process predominantly affects the brainstem, basal ganglia, and frontal lobes, causing the diverse and progressive symptoms observed in PSP patients. The neurodegeneration in these areas results in impaired vertical gaze, postural instability, and various motor and cognitive dysfunctions.
Genetic and Environmental Factors
While the exact etiology of PSP remains unclear, both genetic and environmental factors are believed to contribute. Genetic studies have identified certain haplotypes, particularly within the MAPT gene, that are associated with an increased risk of PSP. Environmental factors, such as exposure to neurotoxins or head trauma, may also play a role, although their exact impact is still under investigation. Research into these factors aims to uncover potential targets for therapeutic intervention and to better understand the disease's underlying mechanisms.
Clinical Presentation and Disease Progression
The clinical presentation of PSP can vary widely among individuals. Early signs often include subtle changes in balance and coordination, leading to frequent falls. As the disease progresses, patients develop more pronounced motor symptoms such as bradykinesia, rigidity, and vertical gaze palsy. Cognitive impairments, including difficulties with executive function, memory, and attention, become more apparent over time. Behavioral changes, such as apathy and depression, are common and can significantly affect the patient's quality of life.
Differential Diagnosis and Overlapping Syndromes
PSP shares several clinical features with other neurodegenerative disorders, making differential diagnosis challenging. Conditions such as Parkinson's disease, multiple system atrophy, and corticobasal degeneration can present with similar motor and cognitive symptoms. Careful clinical evaluation, including detailed neurological examination and neuroimaging, is essential to differentiate PSP from these overlapping syndromes. Accurate diagnosis is crucial for appropriate management and prognosis.
Therapeutic Interventions and Symptom Management
Currently, there is no cure for PSP, and treatment focuses on managing symptoms and improving quality of life. Medications such as levodopa may provide some relief for motor symptoms, although the response is often limited. Other pharmacological treatments, including antidepressants and medications for sleep disturbances, can address specific symptoms. Non-pharmacological interventions, such as physical therapy, occupational therapy, and speech therapy, are essential components of a comprehensive care plan. These therapies aim to maintain mobility, enhance communication, and support daily living activities.
Research and Future Directions
Ongoing research into the pathogenesis of PSP is exploring potential therapeutic targets, including tau protein aggregation and neuroinflammation. Clinical trials investigating tau-targeting therapies, such as monoclonal antibodies and small molecules, are underway and hold promise for altering the disease course. Additionally, research into biomarkers for early diagnosis and disease monitoring is critical for improving patient outcomes. Advances in genetic studies and neuroimaging techniques are also contributing to a better understanding of PSP and its complex pathology.
Support and Resources
Patients with PSP and their caregivers can benefit from various support resources. Organizations such as the CurePSP Foundation and the PSP Association provide educational materials, support networks, and advocacy for those affected by the disease. These organizations also fund research initiatives aimed at finding a cure and improving the quality of life for individuals with PSP. Support groups, both in-person and online, offer a platform for patients and caregivers to share experiences, receive emotional support, and access practical advice.
In conclusion, Progressive Supranuclear Palsy is a debilitating and progressive neurodegenerative disorder that requires a multidisciplinary approach to management. Early diagnosis and comprehensive care, including the use of assistive technologies and therapeutic interventions, are essential for improving the quality of life for individuals with PSP. Ongoing research into the disease's underlying mechanisms and potential treatments offers hope for future advancements in PSP care.
Epidemiology and Demographics
Etiology and Pathophysiology
What causes Progressive Supranuclear Palsy (PSP)?
What does Progressive Supranuclear Palsy (PSP) do to the body?
Clinical Features and Stages
Diagnosis
Diagnostic Criteria
Genetic Testing
Differential Diagnosis
Assistive Technology and AAC Interventions
Communication Devices
Mobility Aids
Access Modalities
Environmental Control Units
Clinical Recommendations
For Speech-Language Pathologists
For Occupational Therapists
For Physical Therapists
For Applied Behavior Analysts
For Special Educators
For All Staff and Caregivers
Care Management
Medical Management
Positioning and Handling
Feeding and Swallowing
Psychosocial Support
Educational Support
IEP Goal Examples
Accommodations and Modifications
Transition Planning
Support and Resources
🏛️ Foundations and Research
🌐 Online Communities
📚 Educational Resources
💰 Financial Assistance
References
Disclaimer: This comprehensive clinical guide is designed for healthcare professionals, educators, and families. For specific medical advice, please consult with qualified healthcare providers.